CAPD Therapy: A New Hope for Kidney Failure Patients Undergoing Dialysis
Blood dialysis therapy has long been synonymous with haemodialysis (HD), which is routinely performed at hospitals. However, kidney failure patients have alternative treatment options, namely Continuous Ambulatory Peritoneal Dialysis (CAPD).
Tony Richard Samosir, Chairman of the Indonesian Kidney Disease Patient Community (KPCDI), stated that most newly diagnosed patients only discover alternative therapies after years of undergoing HD.
“In Indonesia, nearly 98 per cent of kidney failure patients go directly into haemodialysis, whilst other treatment options such as CAPD or transplantation are often not fully explained to patients. For us at KPCDI, this is not merely a matter of treatment methods, but a matter of patients’ rights to obtain complete information and determine their own treatment choices,” Tony stated on Friday (14 March).
Chronic kidney disease (CKD) is often called a silent killer because symptoms are frequently undetectable in early stages. Approximately 90 per cent of patients only become aware of their condition when it has reached an advanced stage requiring dialysis or transplantation. The number of chronic kidney failure sufferers in Indonesia was recorded at approximately 1.5 million patients in 2023 and is estimated to continue increasing.
Amidst this surge, dialysis therapy in Indonesia remains dominated by haemodialysis, with 134,057 patients during the 2022–2024 period. The financing burden borne by BPJS Kesehatan has also increased from Rp6.5 trillion in 2019 to Rp11 trillion in 2024.
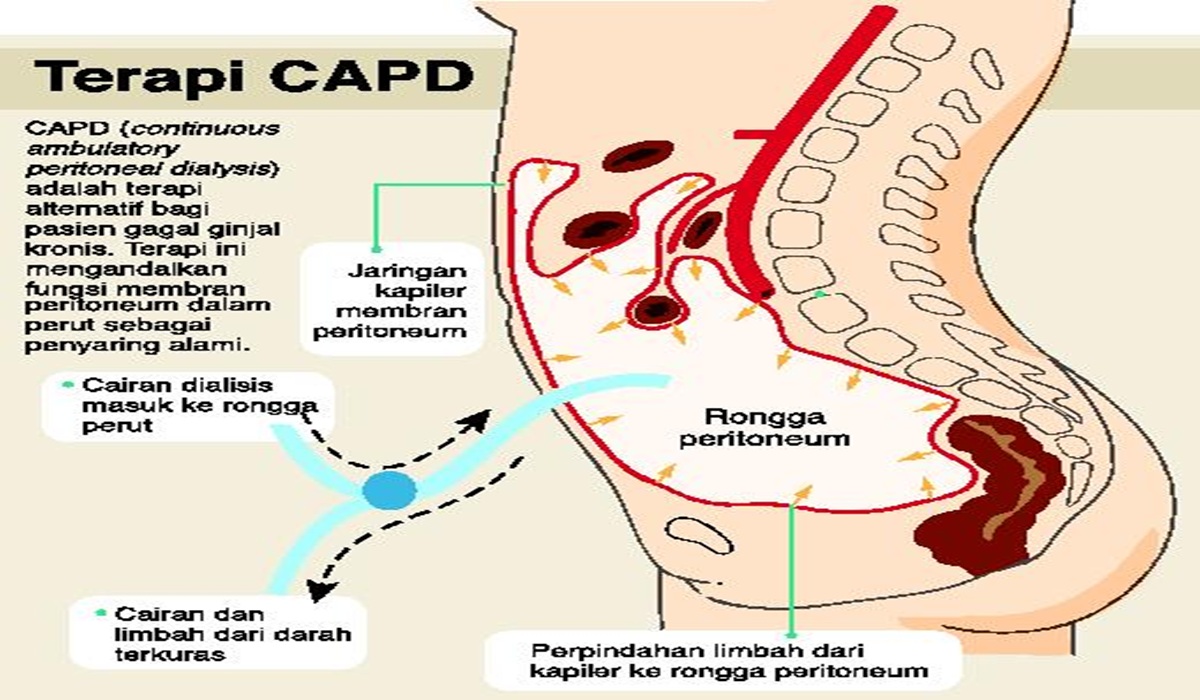
Unlike HD, CAPD allows patients to conduct therapy independently at home by introducing dialysate fluid through a catheter in the abdomen and replacing it three to four times daily. This therapy provides greater flexibility for patients to maintain their activities.
Although covered in the national health system with a tariff of Rp8 million per month in accordance with Health Ministry Regulation Number 3 of 2023, CAPD utilisation remains low. The government targets a minimum of 10 per cent of dialysis patients to use this method.
Tony attributed the low utilisation of CAPD partly to insufficient education regarding treatment options provided to patients from the initial diagnosis. In several countries, he noted, patients are given detailed explanations regarding various treatment options before undergoing dialysis.
“In Malaysia, for example, patients are given detailed explanations regarding both haemodialysis (HD) and peritoneal dialysis (PD) options, so they can determine the most suitable therapy. Meanwhile, in Indonesia, similar education is not yet common,” he said.
He added that after a patient’s condition stabilises following several rounds of haemodialysis, the option to consider CAPD as a continuation therapy is often no longer presented. Consequently, many patients continue with HD because it is the only method they are aware of.
“We frequently hear the same phrase from patients: ‘Why didn’t I know about CAPD from the beginning?’ Many patients only become acquainted with this therapy through patient communities, not from the healthcare system. This demonstrates that education regarding kidney failure treatment options has not been comprehensively communicated to patients from the outset,” he stated.
He hopes that education regarding treatment options becomes part of the standard of care for kidney failure patients so they can understand and determine the most suitable therapy for the long term.
“Kidney failure patients will undergo this therapy for life. Therefore, patients should not merely be objects of treatment, but must be subjects who understand and choose their own therapy,” he concluded.
